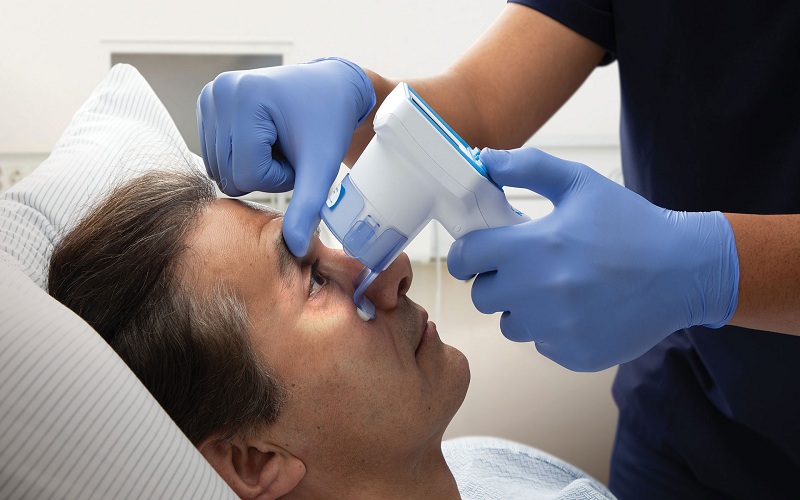
Medical professionals usually see the eyes as a portal through which the inner workings of the body are diagnosed. Apart from the variety of diagnostic tools, there is one that is very useful and interesting: it is to measure the size of the pupils. Physicians can get the bulk of information on their neurological health by merely checking and measuring the dilation of the pupil. This article will cover the importance of assessing pupillary size, describe how it is applied in clinical practice, and identify its contribution to neurological exam improvement.
Applications in Clinical Practice
Pupillary size measure has usage in diverse areas of medicine miscellaneously, but neurology is where it is most important. The pupillary response represents the indispensable marker of neurofunction, reflecting the state of the brainstem and the associated pathways.
For example, in accidental head damage instances, pupillary size measurement can be utilized in evaluating intracranial pressure and neurological status. Anisocoria, which is one of the pupils being smaller than the other one, can be a symptom of an underlying pathology like a brain injury or compression of cranial nerves.
In addition, pupillary abnormalities might also indicate generalized system pathologies as well. Autonomic abnormalities, including Horner’s syndrome and Adie’s pupil, typically present with abnormal pupillary patterns such as dilation or lack of normal response to changes in lighting. By adding pupillary size measurement to the standard examination procedure, clinicians will both shorten the diagnostic process and initiate timely treatment.
Quantifying Changes: Percentage of Pupil Size Change
The measurement of absolute pupil size is useful, but comparing pupil diameter across time provides more diagnostic information. Pupil size % change, calculated by comparing measurements before and after a certain stimulus or intervention, assists doctors in understanding pupillary reactions as dynamic processes.
A pupillary light reflex test, for example, may be administered during a neurological examination by a healthcare professional. By evaluating the percentage change in pupil size in response to light stimulation, doctors may assess the afferent and efferent pathways involved in the pupillary reflex arc. Deviations from typical reactions might suggest nerve injury, neurological diseases, or pharmaceutical effects.
Enhancing Neurological Examinations
While evaluating the nervous system, the precision and accuracy of the test is of the utmost importance. Pupillometry is one of the notable methods to support the standard neuro exam so as to supplement the clinician’s diagnostic armory to have a comprehensive evaluation of the patients.
The neurological Pupil Index (NPI) is one example of the neurological tool, that employs pupil size measurement into a standardized scoring system for the sake of neurological examinations. The Npi algorithm was introduced as part of the Neurological Pupil Index and it assigns numerical values to pupillary parameters based on their deviation from the normal values. By computing and summarizing pupillary irregularities into a single index, the Npi speeds up the process and make an objective and reproducible assessment of neural deficiencies possible.
Moreover, recent technological advancements have brought about novel techniques for the measurement of these parameters, thereby increasing precision and productivity. Automatic pupillometers integrated with intensity spectral cameras and the development of algorithm analysis would help in measure pupil size and real-time measurements, having minimal human errors and standardizing the evaluation process.
Challenges and Considerations
While being useful, this measurement method also contains some disadvantages and problems. The fluctuation of pupil size is common throughout the human race and is known as physiological anisocoria. It may, therefore, lead to misinterpretations, and the case of baseline measurements must be taken into account. Moreover, variables like age, drugs, and the surrounding environment can affect the size and response of the dilator muscle, which makes the clinicians incorporate their findings into the broader context.
In addition to the fact that oculography gives a lot of information for diagnostics, there is no need to limit the examination to the measurement of pupil size only. Combining pupillary examinations together with other clinical evaluations, imaging studies, and laboratory tests will improve an accurate estimation of the situation and contribute to an appropriate treatment plan.
Conclusion: Illuminating Insights
In the medical space, diagnostic pupillometry has a well-deserved role as a reliable and diverse tool assessing the central neurological function status. The eyes have it! They can tell us about the slightest idiosyncrasies, from brain injury to the most complicated autonomic dysfunction tangle.
Healthcare practitioners may enhance patient outcomes, accelerate therapies, and strengthen their diagnostic skills by leveraging the knowledge gained from pupillary size assessment. As our understanding of pupillary reactions grows, so will our capacity to use this vital diagnostic tool for human health.